Systematic Review of Conversion of Total Shoulder Arthroplasty to Reverse Shoulder
David Southward Constantinescu, Department of Orthopedic Surgery, University of Miami, USA.
Abstract
Background: The purposes of this study were to determine the average fourth dimension from hemiarthroplasty (HA) or total shoulder arthroplasty (TSA) to conversion to contrary total shoulder arthroplasty (RTSA) and to determine the factors leading to conversion to RTSA.
Methods: A review of the literature regarding the existing bear witness for conversion of HA/TSA to RTSA was performed. Inclusion criteria were as follows: reporting of conversion of a HA or TSA to RTSA with a follow up of greater than 24 months, English language, and human being studies. Excluded were articles that did not mention a time to conversion surgery.
Results: I hundred studies were initially retrieved with iii meeting the inclusion criteria. The weighted mean time to conversion of HA/TSA to RTSA was 36.eight months. Rotator gage failure was the indication for conversion in 66% of cases (65/99), while component loosening (glenoid or humeral stem) was the indication in 14% (xiv/99) of cases.
Conclusions: Amidst patients that undergo conversion of HA/TSA to RTSA the reported time to conversion was 36.viii months on average. The most mutual indication for conversion to RTSA was rotator cuff failure, highlighting the importance of rotator gage integrity when performing a primary HA or TSA.
Keywords: Shoulder, arthroplasty, total shoulder arthroplasty, reverse shoulder arthroplasty, rotator gage tear, revision shoulder arthroplasty, conversion shoulder arthroplasty.
Abbreviations:
1.Hemiarthroplasty (HA).
2.Total shoulder arthroplasty (TSA).
3.Reverse full shoulder arthroplasty (RTSA).
Introduction
The number of primary total shoulder arthroplasty (TSA) procedures performed is increasing [1-3]. The demand for conversion to reverse total shoulder arthroplasty (RTSA) tin likewise expected to follow given the number of principal TSAs performed among an increasingly active population. In instances of TSA or hemiarthroplasty (HA) where anatomic revision is not possible, a RTSA may be indicated to provide biomechanical stability to the shoulder [4-vii]. No registrar information or aggregate literature assay currently exists on the time from HA or TSA to conversion to RTSA.
There were ii purposes of this written report. The chief purpose of this study was to determine the boilerplate time from HA/TSA to conversion RTSA. The secondary purpose of this report was to determine the factors leading to conversion to RTSA. The outcomes of a revised TSA can be predicted on whether the indication for revision a component-related problem or soft tissue deficiency is [viii] Therefore, surgeons must be aware of the nearly mutual reasons for HA/TSA revision and accept this into account into their planning and prognostic discussions with patients. Our hypothesis was that the about common indication for conversion to RTSA was rotator gage insufficiency.
Materials and Methods
Article Identification and Pick
This study was conducted in accordance with the 2009 Preferred Reporting Items for Systematic Review and Meta-Assay (PRISMA) statement. A systematic review of the literature regarding the existing bear witness for conversion to RTSA was performed using the Cochrane Database of Systematic Reviews, the Cochrane Central Register of Controlled Trials, PubMed (1980-present), and MEDLINE (1980-present). The queries were performed in August 2019.
The literature search strategy included the following search: "(((total shoulder arthroplasty) OR full shoulder replacement) AND conversion". Inclusion criteria were as follows: reporting of conversion of a HA or TSA to RTSA with a follow up of greater than 24 months, English language, and human studies. The exclusion criteria included: non-English articles, instance reports, technique papers, and articles that did not mention a fourth dimension to conversion surgery. All references within included studies were crossreferenced for inclusion if missed by the initial search. If a duplicate report population was encountered, the manuscript with the longer mean follow-up was included to avoid overlap.
Two investigators independently reviewed the abstracts from all identified manufactures. Full-text articles were obtained for review if necessary to let further assessment of inclusion and exclusion criteria. Additionally, all references from the included studies were reviewed and reconciled to verify that no relevant articles were missing from the systematic review.
Bias
Studies classified every bit level of bear witness 3 or iv can potentially be affected by selection and performance bias because of the lack of randomization and prospective comparative control groups (level 4), especially in populations characterized by heterogeneity of injuries. Selected studies were reviewed to ensure that authors minimized bias while recognizing the constraints present with such studies.
Data Collection
The level of evidence of the studies was assigned co-ordinate to the classification equally specified by Wright et al. [9] The information was collected from the included studies. Patient demographics, follow-up, event scoring methods, primary surgery, fourth dimension to conversion surgery and implant organisation used were extracted and recorded. For continuous variables (eg, age, timing, follow-upwards, outcome scores), the hateful and range were collected if reported. Information were recorded into a custom Microsoft Excel spreadsheet (Microsoft Corp) using a modified information extraction table.
Results
Study Selection
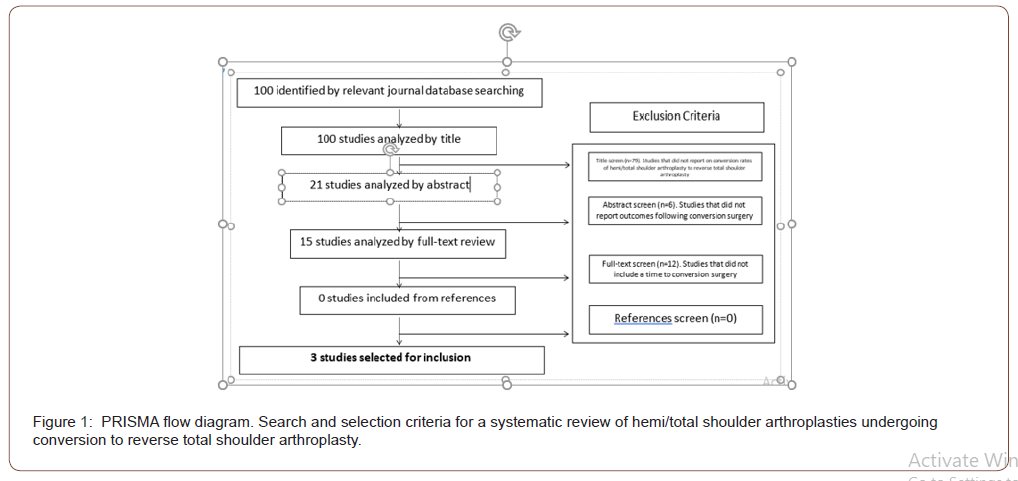
The systematic search performed using the in a higher place-mentioned keywords and phrases identified three studies, after removing duplicates and applying exclusion criteria [10-12]. One hundred articles were initially identified from the MEDLINE database. There were no boosted manufactures from the Cochrane database. Each commodity was first screened by title leaving 21 manufactures. Excluded articles based on title screen were those that did not study on conversion surgeries from HA/TSA. The remaining articles were then screened by abstruse yielding 15 articles. Excluded articles based on abstract screen were those that did non report outcomes following conversion surgery. Afterward full text review, three studies met criteria and were included in the review. Studies that were excluded subsequently full text screen were those that did not report a time to conversion surgery from primary surgery. Two studies that were included were of Level III evidence and one study was of Level IV evidence. Figure ane is a PRISMA flowchart that demonstrates option criteria of the systematic review. Following review of all references from the included studies, no additional studies met inclusion criteria.
Demographics
In this review a total of 99 patients were included. Written report sizes ranging from 17 patients to 56 patients. The review included 99 patients (31 male, 68 female) with a mean age 69 (range: 67 – 73). The average follow up was 35.8 months (range: 32.3 – 37.4). Demographics of each included study are reported in Tabular array i.
Table i:Study design, patient demographics and result scores of included conversion RTSA studies. VAS = Visual analog scale.
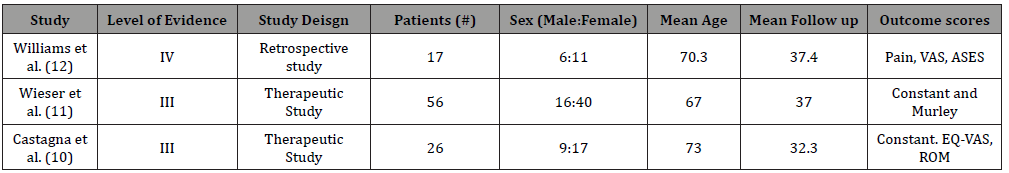
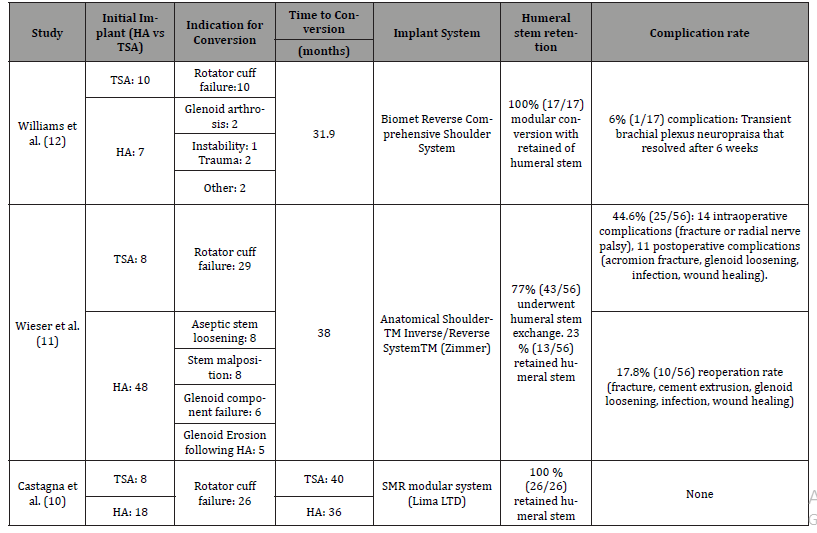
Table 2:Primary surgery implant, indication for conversion, time to conversion, implant organization, retention of master humeral stem and complication rates for included conversion RTSA studies. HA = hemiarthroplasty. TSA = total shoulder arthroplasty.
Fourth dimension to conversion RTSA
The weighted mean time to conversion of HA/TSA to RTSA was 36.eight months (31.9 – 40). Individual times reported by each study are detailed in Table 2. All three studies contained patients whose principal surgery was a HA or TSA. Castagne et al. was the simply of the iii who compared the time to surgery between HA and TSA [x].
Indications for Conversion
Rotator gage failure occurred in 66% of cases (65/99), while component loosening occurred in fourteen% (14/99) of cases. Among the component loosening, glenoid occurred in vi% (6/99) of cases and humeral stem occurred in 8% (8/99) of cases. Castagne et al. reported that 100% (26/26) patients who underwent conversion did and so due to rotator gage insufficiency [10]. None of the studies reported evaluation of rotator cuff integrity prior to primary TSA.
Chief surgery hardware retention and complication rates
Retaining the humeral stem when performing RTSA conversion surgery occurred in 57% (56/99) of patients. Humeral stem substitution was performed in 43% (43/99) of patients. All three studies reported on complications. Overall, in that location was a 26.2% (26/99) complication charge per unit among conversion RTSA's. Reoperation rate was x% (10/99) and all reoperations occurred inside Wieser et al. [xi].
Discussion
This review constitute that the reported time to conversion of HA/ TSA to RTSA was 36.8 months on average with the most mutual indication for conversion being rotator cuff insufficiency. This highlights the importance of rotator cuff integrity when performing a master HA or TSA.
TSA has historically been indicated in patients with pain due to isolated glenohumeral arthritis while RTSA has been indicated in cases of rotator cuff arthropathy [13]. Survivorship studies have demonstrated that 85% of primary TSA's will survive 20 years, with the most common demand for revision beingness component loosening. [xiv] However, restoring range of motion and activity in previously arthritic shoulder may predispose the rotator cuff to damage. The resultant loss of function in the shoulder may be addressed through conversion of a TSA to RTSA, which recovers shoulder role through restoring the deltoid muscle and altering the functional fulcrum in a rotator cuff deficient shoulder [15]. In fact, a recent study has suggested that RTSA's may take a role over TSAs in select populations with glenohumeral arthritis even in the presence of an intact rotator gage [xvi]. Our study corroborates this idea given the high incidence of rotator gage insufficiency that necessitated conversion to RTSA.
Due to anticipated rotator cuff insufficiency that may follow TSA, modular components of the humeral stem and glenoid have been designed to facilitate conversion to RTSA [17-twenty]. Retaining the humeral stem when performing conversion RTSA has been demonstrated to result in lower complication rates [21-24] Of the three studies included in our review, Wieser et al was the only ane to include a accomplice of patients undergoing humeral stem exchange and also plant that stem substitution was associated with a college complexity charge per unit than stem retention [11].
Complexity rates for RTSA take been reported to be approximately xv% in the principal surgery and become higher (40%) when RTSA in the revision setting [25]. The complexity rate in our studies was 26.ii% (26/99) rate among conversion RTSA's, with the majority of complications existence from a cohort of patients that included humeral stem exchange. This finding emphasizes the importance of proper component alignment in the primary surgery to minimize complications if a revision surgery is required.
An important limitation of this study was the level of evidence of the included studies. All were Level III or Iv of retrospective cohorts of patients. Afterward, it is hard to give definitive quantification of arthroplasty longevity and predisposing factors to revision surgery. Being that not all main HA'southward TSA'due south were included and followed for an extended period, this was non a survivorship study suited to respond how long HA/TSA final. Rather, we were able to provide insight as to when principal HA/TSA'south are typically converted to RTSA and the underlying etiology necessitating revision. Based upon bachelor literature, this manuscript is able to provide reasonable analysis to aid the dr. in prognostic factors in conversion RTSA.
Conclusions
Among patients that undergo conversion of HA/TSA to RTSA the reported time to conversion was 36.eight months on boilerplate. The most common indication for conversion to RTSA was rotator cuff failure, highlighting the importance of rotator gage integrity when performing a primary HA or TSA.
Disharmonize of Interest
The authors, their firsthand family, and whatever research foundation with which they are affiliated did not receive whatsoever financial payments or other benefits from any commercial entity related to the subject of this article.
The authors, their firsthand family, and any research foundation with which they are affiliated did non receive any grant sport or research funding.
Acknowledgement
None.
campbelllationd1950.blogspot.com
Source: https://irispublishers.com/arar/fulltext/time-to-conversion-of-hemitotal-shoulder-arthroplasty-to-reverse-total-shoulder-arthroplasty.ID.000517.php
0 Response to "Systematic Review of Conversion of Total Shoulder Arthroplasty to Reverse Shoulder"
Post a Comment